Hard palate foreign body removal in the pediatric population.
Foreign body ingestion is a common problem in the pediatric population, but foreign body adherence to the hard palate is reported less frequently. Particular challenges in the pediatric population include the frequent lack of a clear ingestion history, inability to communicate symptoms well, and difficulty of obtaining a thorough examination or attempt at removal in very young children.
The majority of reported foreign body ingestions consistently occur in children less than or equal to five years old. [1,2] Coins, followed by small sharp objects and batteries, are the most commonly ingested items. [3] Foreign bodies adhered to the hard palate are seen less frequently.
It has been hypothesized that increased intraoral pressure from feeding and pacifiers may help increase the seal of the object on the hard palate.[4] This may be why foreign bodies adhered to the hard palate are not swallowed and remain asymptomatic initially.
We present a case of unusual foreign body adhesion to the roof of mouth and discuss effective evaluation and treatment and a differential diagnosis.
Case Presentation
The patient is a 17-month-old Caucasian male who presented with a black and white mottled lesion on the roof of his mouth. Parents noticed it when he was laying on the ground crying after a sibling had taken a toy from him. Previously, he was eating and drinking normally, and not in any apparent pain or distress.
He had not had fevers, decreased appetite or activity, night sweats, weight loss, respiratory distress, abnormal breathing or rash. He was teething and had no history of palatal defects. Patient was seen two months before at the pediatrician’s office, and no abnormalities were noted. Parents recalled that the patient was found eating dirt recently, and that they were renovating their home, including a shower remodel.
Patient had a history of mild eczema. He was up to date on immunizations and did not take medications. He had no known allergies and no surgical history. Family history included one family member with a history of melanoma. Patient lived at home with mother, father and two siblings.
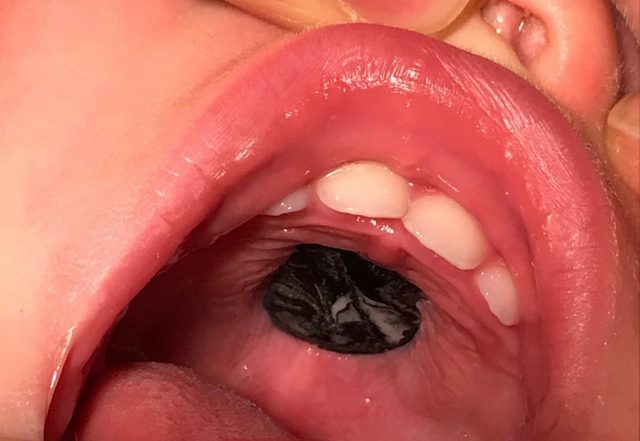
On examination, patient was well-appearing, afebrile and not in respiratory distress. On the most superior aspect of the hard palate, there was a smooth, hard mass, flush with surrounding tissue. It was predominantly black with a white marbling effect and was not tender to touch or friable.
There was no surrounding erythema, and the density was similar to that of the hard palate. It was adhered to the surrounding tissue and could not be easily dislodged with a gloved finger (figure 1).

Foreign body adhered to the hard palate in situ.
There was otherwise normal oropharyngeal anatomy without trauma. There was no cervical lymphadenopathy or masses, stridor, tachypnea or retractions. Patient did not have focal neurologic deficits, lesions, rashes or nevi. Differential diagnosis included foreign body, melanotic nevus, melanotic neuroectodermal tumor of infancy, angiomyolipoma, mucous cyst, eosinophilic granuloma, sarcoma or leukemic infiltrate.
An otolaryngologist was consulted and after evaluating the child under moderate sedation, was able to successfully remove the lesion intact with a right-angle probe. The underlying palate was not discolored, ulcerated or injured. The mass was determined to be a piece of black dyed, white epoxy (figure 2).

Piece of epoxy after removal.
It was most likely ingested from excess drippings on the floor the family’s shower renovations, which was being remodeled with an epoxy substance to seal the edges. In retrospect, they recalled the child crawling around in the area two days before. It is most likely that the patient put a soft piece in his mouth, which then molded to the roof and smoothed down with his tongue.
Discussion
In the pediatric population, diagnosing a foreign body can be challenging due to an often lack of a clear ingestion history, inability to communicate symptoms, and patient intolerance of a thorough examination.
Due to these challenges, evaluation under sedation may be a necessary first step. A right-angle probe or other curved pick can be successfully used to both diagnose and therapeutically remove hard palate foreign bodies, saving the patient from unnecessary advanced imaging, laboratory studies, general anesthesia, and trauma secondary to multiple examinations.
Prolonged adhesion of foreign bodies allows inflammatory growth in the underlying and surrounding mucosa, and may increase the degree of difficulty to remove over time. Similar hard palate foreign bodies have been reported with removal in the operating room.[5–7]
It is important that foreign bodies remain high on the differential in young children with intraoral or hard palate lesions, even without a clear history of trauma or ingestion, as they are significantly much more common than other oral lesions in this population.
Misdiagnosis can result in unnecessary workup, cost and potential harm. Evaluation and therapeutic removal with a right-angle probe, with or without sedation, is a safe, effective way to evaluate and manage this condition.
References
- Bronstein AC, Spyker DA, Cantilena LR, Rumack BH, Dart RC. 2011 Annual report of the American Association of Poison Control Centers’ National Poison Data System (NPDS): 29th Annual Report. Clin Toxicol (Phila). 2012;50(10). doi:10.3109/15563650.2012.746424
- Gummin DD, Mowry JB, Spyker DA, Brooks DE, Osterthaler KM, Banner W. 2017 Annual Report of the American Association of Poison Control Centers’ National Poison Data System (NPDS): 35th Annual Report. In: Clinical Toxicology. Vol 56. ; 2018. doi:10.1080/15563650.2018.1533727
- Arana A, Hauser B, Hachimi-Idrissi S, Vandenplas Y. Management of ingested foreign bodies in childhood and review of the literature. Eur J Pediatr. 2001;160(8). doi:10.1007/s004310100788
- de Jong A., Moola F, Kramer D, Forte V. Foreign bodies of the hard palate. Int J Pediatr Otorhinolaryngol. 1998;43(1). doi:10.1016/s0165-5876(97)00152-3
- Ondik MP, Daw JL. Unusual foreign body of the hard palate in an infant. J Pediatr. 2004;144(4). doi:10.1016/j.jpeds.2003.09.038
- Adeyemo WL. Foreign body impaction aided by thumb-sucking in the palate of an infant. J Craniofac Surg. 2012;23(4). doi:10.1097/SCS.0b013e31824dfb66
- Rasband-Lindquist AN, Lusk R. Unusual hard palate foreign body: A case report. Ear, Nose Throat J. 2013;92(4). doi:10.1177/014556131309200423