Breaking down the various causes of the oral mass.
A 38-year-old African American male presented to the emergency department with an oral mass. He was struck on the mouth by a wrench handle about two years ago and since then has had a growing mass originating from the gingiva of his left front upper teeth. He had not sought medical care since his original injury, but was no longer able to eat solid foods and had to use a straw for all PO intake. The patient denied fevers, chest pain, shortness of breath or weight loss. He had no significant past medical history and denied tobacco, alcohol or illicit drug use.
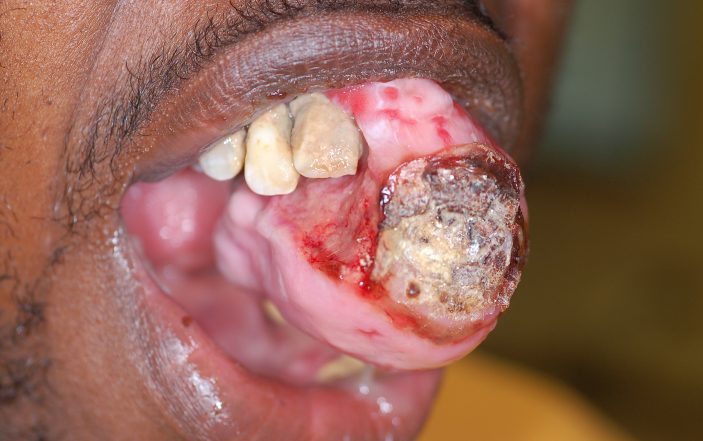
Physical exam in the emergency department revealed an alert male in mild discomfort, but no acute distress. Vital signs were: Temp 36.9 °C, 152/92, HR 106, RR 16, Pulse Ox 100% on room air. Oral exam revealed a large 4x3cm firm, oozing growth on the premaxilla with necrotic material on the anterior aspect with ulceration (figures 1-3).
 The patient had poor dentition, but there was no fluctuance or halitosis. His neck was supple without adenopathy. Cardiac and pulmonary exams were unremarkable.
The patient had poor dentition, but there was no fluctuance or halitosis. His neck was supple without adenopathy. Cardiac and pulmonary exams were unremarkable.
No laboratory data was obtained.

ENT was consulted and requested a facial CT that identified a soft tissue mass in the anterior mouth, whose epicenter appeared to be at the left maxillary incisors (figure 4). This undifferentiated oral mass was of a significant enough size to affect the patient’s ability to eat. However, he was tolerating his secretions and had no evidence of airway compromise. Therefore, it was not considered an emergency, and he was referred to outpatient ENT. Subsequently, he was admitted for resection of the mass without any complications. He had two post-op visits that revealed the surgical site was healing well with good cosmetic outcome.
Discussion
This patient had an ossifying fibroid epulis that was diagnosed on CT and confirmed by surgical pathology. Also known as peripheral ossifying fibroma, it is believed to be caused by irritants or trauma (as in the case of this patient). The prevalence is greatest in teenagers and young adults with the majority of cases occurring in females.
Lesions are sessile or pedunculated, typically ulcerated, color ranging from red to pink, and are usually <3cm in size. They tend to grow on the maxilla and around the incisors. Microscopic examination will show mineralized components with fibrous proliferation. The mineralized portion can consist of bone, cementum or dystrophic calcifications. More mineralization tends to be present when the epulis has existed for a longer period of time.
Treatment consists of complete surgical excision and aggressive curettage of adjacent tissues. Recurrence rate has been reported up to 20% and probably occurs due to incomplete removal, repeated trauma or persistence of the irritants. Our patient didn’t have any additional visits after his post-op visits, therefore it is unknown if he had any recurrence.
An epulis is a benign growth on the gingiva or alveolar mucosa. The term only describes the location of the growth and has no further implications on the nature of the lesion. There are various types of epulis depending on the components or etiology: epulis fissuratum, epulis granulomatosum, congenital epulis, pregnancy epulis, giant cell epulis and ossifying fibroid epulis. The definitive treatment for any epulis is surgical excision.
Epulis fissuratum is fibrous hyperplasia that develops in response to chronic irritation from a poor fitting denture. This condition is most common in the elderly, since this population is more likely to be edentulous and to wear a denture, and in women. Epulis fissuratum typically develops along the anterior portion of the alveolar ridge. The lesions appear as firm, pink folds of tissue adjacent to a denture flange with occasional erythema and ulceration particularly at the bottom of the groove. Treatment is surgical excision followed by relining of the denture to prevent recurrence.
An epulis granulomatous, a variant of pyogenic granuloma, is a benign hyperplastic growth that arises from a recently extracted tooth socket. Following a tooth extraction, healing of the socket occurs by regeneration of epithelial and connective tissue with replacement of space by fibrovascular tissue. The sharp bony spicules of the alveolar wall or tooth structure can act as triggers for an inflammatory reaction that inhibits healing.
To prevent the formation of an epulis granulomatosum, the removal of any bony spicules or tooth fragments at the time of extraction must be performed. With ongoing inflammation and persistence of the precipitating agents, hyperplastic tissue develops along with proliferative blood vessels to result in formation of a mature fibrous stroma.
Clinically, it is characterized by a reddish, smooth, sessile or pedunculated, nontender, rapidly growing mass. The lesion often bleeds easily because of its high vascular content. The treatment is complete excision and curettage of the socket floor to ensure the elimination of irritating particles is needed to prevent recurrence.
Congenital epulis is a rare epulis that presents at birth. It is an exophytic benign tumor that arises from the alveolar ridge of the maxilla and mandible. The etiology of the tumor is unclear but has a female predominance ratio of 10:1. The lesions are usually pink, pedunculated, firm and have a smooth or lobulated surface. The size varies from a few mm to 2 cm. They are usually found in solitary with multiple growths only in 10 percent of cases.
Rarely does the epulis interfere with feeding or breathing. Congenital granular cell epulis stops growing at birth, occasionally regressing spontaneously. Although monitoring for regression may be an option, the definitive treatment is surgical excision and is especially necessary if the lesion interferes with respirations or feeding.
A rare epulis that develops only in pregnancy is called epulis gravidarum or pregnancy epulis. This lesion is identical to a pyogenic granuloma in all aspects except that it only occurs during pregnancy. It is a benign lesion of the gingiva, particularly the interdental papillae.
Clinically, it is usually soft, pink or red, smooth or lobulated, vascularized, exophytic growth on a pedunculated or sessile base that develops over a few days to weeks typically during the second or third trimester. It is thought to arise in response to hormonal changes that trigger a gingival inflammatory to dental plaque. Spontaneous resolution usually occurs postpartum; therefore, no intervention is typically performed for small lesions. Larger lesions may require excision.
Giant cell epulis, also known as peripheral giant cell granuloma is an overgrowth of tissue due to irritation or trauma. The lesion arises from the periodontal ligament enclosing the root of a tooth. The usual age at diagnosis is the fourth through sixth decades and has a 60 percent gender predilection for females.
The lesions are nodular and pedunculated, frequently have an ulcerated surface, with a reddish to bluish hue. They can grow quickly and exceed 4cm in size, but usually remain less than 2cm in diameter. Histologically, multinucleated giant cells are seen in a background of mesenchymal cells and extravasated red blood cells. Treatment consists of complete surgical excision and extensive cleaning of any adjacent teeth to removal all giant cell tissue. A recurrence rate of 10% has been reported.

Figure 4: CT face: soft tissue mass in the anterior mouth, whose epicenter appears to be at the left maxillary incisors. This mass demonstrates areas of cloud-like calcification and measures approximately 6.6 x 4.2 x 3.3cm. There is erosion of the left maxillary alveolus.
References:
https://dermnetnz.org/topics/epulis/
https://www.sciencedirect.com/topics/medicine-and-dentistry/epulis
https://www.researchgate.net/publication/307699664_Recurrent_epulis_granulomatosa_A_second_look – Manovijay B, Rajathi P, Fenn SM, Sekar B. Recurrent epulis granulomatosa: A second look. J Adv Clin Res Insights 2015;2:140-142
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5516740/
Mortazavi H, Safi Y, Baharvand M, Rahmani S, Jafari S. Peripheral Exophytic Oral Lesions: A Clinical Decision Tree. Int J Dent. 2017;2017:9193831. doi:10.1155/2017/9193831
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4774304/#ref13
Kumar RM, Bavle RM, Umashankar DN, Sharma R. Congenital epulis of the newborn. J Oral Maxillofac Pathol. 2015;19(3):407. doi:10.4103/0973-029X.174642
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4245672/
Abu Gharbyah AZ, Assaf M. Management of a Peripheral Giant Cell Granuloma in the esthetic area of upper jaw: A case report. Int J Surg Case Rep. 2014;5(11):779–782. doi:10.1016/j.ijscr.2014.09.014

3 Comments
Nice case! Are there any pictures post-op?
–> pics or it didn’t happen 🙂
The United States is one of the wealthiest countries and the world, and this human wasn’t able to get help for this issue until he couldn’t eat and ended up in the ER. Shame on us.
NP: I sympathize w/you; but, do you know that he’d attempted to get help for it?