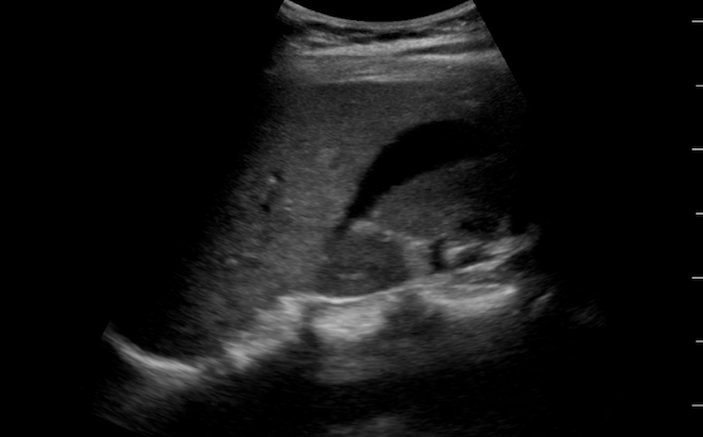
A 28-year-old female passes out at home after a day of increasing abdominal cramping. What can you learn from this ultrasound?
“Hey, I think I see an elephant.” Your trusty resident exclaims as she briskly wheels the ultrasound machine out of the patient’s room. Noting the spring in her step, you walk quickly over to her and ask her to tell you about the patient she just evaluated.
“The patient is a 28-year-old G4P4 healthy female who presented to our ED with abdominal pain and syncope. She was at home earlier today when she noticed she was having increased abdominal cramping. This progressed throughout the day and about 20 minutes ago, she passed out. Her significant other called 911 and EMS arrived within minutes. En route, she had a blood pressure of 65/palp and she was tachycardic to 120 bpm. They placed a large bore peripheral IV and gave her a 2L normal saline bolus.”
As your resident is summarizing the case, you are thankful to see out of the corner of your eye that your nurses are drawing a rainbow of blood tubes, including a pink top for a type and screen.
Your resident begins pulling up her ultrasound images as she continues “When the patient arrived, her blood pressure had improved to 92/56 and her heart rate was down to 98 bpm. I performed a scan of her pelvis and right upper quadrant and these are the images I got.
- What do you see in Figure 1 and Figure 2?
- What is in your difgerential diagnosis for this patient?
- What are the next best steps in management?
- Slide back and forth to see the results in Figure 3 and Figure 4.




As you are reviewing the images with your resident, one of your favorite nurses joins the conversation. “I guess that sort of looks like an elephant to me, too” he quips.
Your resident punches him in the shoulder and explains, “Haven’t you ever heard of the elephant test? It refers to something that is hard to describe, but you know when you see it. I have no idea what I’m looking at right now, but I know it is not normal…”
Your resident continues, “So, the story gets even more complicated. The patient had a baby three months ago via normal spontaneous vaginal delivery and she has been breastfeeding. She had an elective laparoscopic bilateral salpingectomy a month ago. She denies any trauma and she has no other medical history or health issues. When I first read her triage note, I immediately thought about a ruptured ectopic pregnancy. What the heck am I looking at on her ultrasound?”
You pause for a minute to make sure your staff is running a quick point-of-care pregnancy test and that OB/Gyn has been paged emergently to the ED. Luckily, the consult team was already in another part of your ED finishing up another patient. They walk over to join your discussion as you help everyone decipher the ultrasound images.
The patient has an anechoic stripe of free fluid in Morison’s pouch in the right upper quadrant (Figure 3).
Her pelvis views show an empty uterus with a normal, hyperechoic, white endometrial stripe. She has a heterogeneous mixture of clotted blood surrounding her uterus in the anterior and posterior cul-de-sacs and around the fundus of her uterus. It also appears as if she has a left sided ovarian cyst. (Figure 4)
Your astute OB/Gyn consult recognizes that the patient needs to be taken to the OR immediately and that there is no reason to delay surgery and definitive surgical treatment. In the absence of trauma, her intra-peritoneal bleeding is likely from a ruptured hemorrhagic cyst, ruptured ectopic pregnancy, or complications from her recent surgery. As the patient is being wheeled out of the ED, the point-of-care pregnancy test comes back negative.
A few hours later, your OB colleagues stop by to give you an update on the patient. In the OR, the patient was found to have 1500 mL of blood in her peritoneum. Some of it had clotted in her pelvis, but the blood in her right upper quadrant appeared fresh and liquefied. She had denuded serosa and raw tissue that was bleeding at the site of her recent salpingectomy near her uterine cornua bilaterally. And, yes, she also had a left ovarian cyst.
“That was a great pick-up you and your resident made with bedside ultrasound.” Your OB colleague says as she pats you on the back. You accept her praise with a warm smile and respond “I love our job. Especially on days when elephants turn out to be zebras.”
PEARLS & PITFALLS FOR POINT-OF-CARE PELVIC ULTRASONOGRAPHY
- Females with abdominal pain can be diagnostically challenging because of the various organs that could be causing the patient’s symptoms. Use bedside ultrasound to augment your clinical findings and to help expedite care.
- Do not send an unstable patient to radiology. Perform a bedside, point-of-care ultrasound to assess for intra-abdominal free fluid or hemoperitoneum during your initial assessment.
- Any patient with a positive pregnancy test and free fluid visible on bedside ultrasound should be suspected of having a ruptured ectopic pregnancy until proven otherwise. In some ectopic pregnancies, free fluid is the only sonographic abnormality appreciated.
- Think about other etiologies other than ectopic pregnancy that can cause intra-abdominal bleeding in female patients (e.g. trauma, ruptured ovarian cysts, post-procedural bleeding, etc.)
- Include a scan of the hepatorenal recess (Morison’s Pouch) in patients that you are concerned about intra-peritoneal hemorrhage. This is one of the most dependent parts of the body when the patient is lying supine and free fluid may be clearly visible in Morison’s Pouch.
- If Morrison’s Pouch is clean, evaluate the pelvis via a transabdominal approach. Fresh blood will appear as a dark black anechoic or hypoechoic stripe in the posterior cul-de-sac or retrouterine space.
- As more bleeding occurs, and blood accumulates in the pelvis, you will start to note blood collect in front of the uterus in the anterior cul-de-sac, as well.
- As blood begins to clot, it will become more hyperechoic on ultrasound. Fresh blood will appear as dark black anechoic lines swirling around the hyperechoic collections of clotted blood.
- Always assess the uterus for the presence or absence of an intrauterine pregnancy, and have a pregnancy test running while you are scanning the patient.