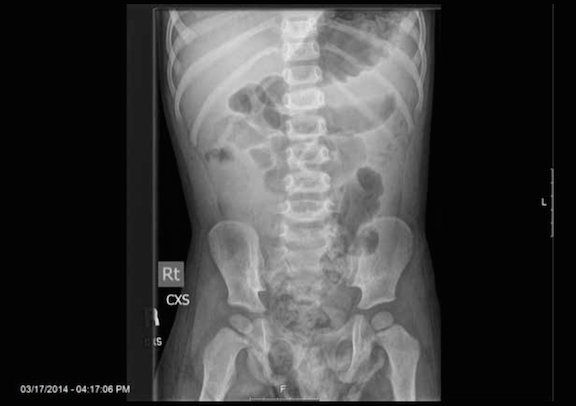
Is this child’s pain all from a fall down the stairs?
A 23-month-old male presented to the emergency department with vomiting, abdominal pain, limp, left hip and leg pain. Eight days prior to presentation the child accidentally fell down a flight of six uncarpeted stairs. He slid down on his belly with no apparent injuries. He subsequently complained of left sided lower leg pain and difficulty walking. He was taken to a local urgent care center where he was diagnosed with non-specific leg pain.
One day later he was taken to a local emergency room with persistent abdominal pain, vomiting and limp. The emesis was non-bilious, non-bloody, and non-projectile and there was no diarrhea or constipation. There was no history of any fever or recent travel, sick contacts and no ingestion of raw meat or any unusual food. In addition, the parent’s stated that he was not walking and would not bear weight on left leg since the fall.
Past History
Significant for a femur fracture at age 4 months, for which he was evaluated and was attributed to be due to non-accidental trauma (NAT). Per mom the county had given back the custody to them.
Physical Exam
Temperature 36.7 C, pulse 118 bpm, respirations 32/minute, BP 130/90mm Hg (agitated), pulse oximetry 97% on room air, and a weight 13.2 Kg. The child appeared comfortable with mom but cried on exam. Head examination was atraumatic. His neck was supple and nontender. The ears, nose, throat and eye exam was normal. Heart sounds were normal with no murmurs. His abdominal exam was equivocal: there was minimal diffuse tenderness but a crying and screaming toddler made the exam difficult. He did not have any peritoneal signs and his bowel sounds were normal. Neither palpable organomegaly nor a mass was identified. A very faint bruise was noted on the right upper quadrant and was from the fall off stairs 8 days ago per mom. Genital exam was normal. He was moving his legs while on the stretcher on mom’s lap and with a normal passive movement. There was no swelling, redness, deformity of his lower extremities. All limbs were warm and well perfused. There was no hip, knee, ankle, and foot tenderness on examination. With ambulation he would limp and not bear weight on his left leg.
Laboratory results demonstrated a mild leukocytosis with a normal hematocrit and platelet count; serum bicarbonate was 18 mmol/L, Glucose 78 mg/dL; normal LFT’s; Serum Amylase 500 U/L, Lipase 893 U/L; Urinalysis showed 3+ ketones but no evidence for infection; C-reactive protein level was 8.63 mg/dL (Normal <0.8mg/dL) and ESR 34 mm/hour.
Abdominal radiographs demonstrated mildly dilated loops of small bowel with concerns for ileus versus early obstruction (Figure 1 above title: abdomen x-ray from outside hospital); Pelvis X-Ray was negative for dislocation or fracture. Abdominal ultrasound from the outside hospital demonstrated evidence of free fluid in the left lower quadrant with no sonographic evidence of intussusception. Liver, spleen and gall bladder were normal. The visualized portions of pancreas were normal.

Figure 2: CT scan of the Abdomen showing the pancreatic pseudocyst
CT Abdomen and Pelvis with contrast: (figures 2, 3) was obtained with the initial read by the over-night radiology resident as: “Scattered amount of free fluid noted in the peritoneal cavity, in the perihepatic region and in the pelvis. Large amount of contents noted in the stomach. No evidence of small or large bowel obstruction.”

Figure 3: Large pancreatic pseudocyst on CT scan on day of admission
The child was transferred to the pediatric hospital and admitted for an intra-abdominal pathology likely related to abuse. The final and confirmatory diagnosis was made the following day when the CT scan was read by a pediatric attending radiologist as “pancreatic pseudocyst with pancreatic laceration probably due to non-accidental trauma (figure 4, CT abdomen and pelvis after 5 days from admission).

Figure 4: Repeat scan 5 days after admission: Enlarging pancreatic pseudocyst. (13.6 x 11.7 x 9.2)
Discussion
Pancreatic pseudocyst is an uncommon pediatric illness caused by pancreatitis or pancreatic trauma, the latter the most common cause in children. Pseudocyst associated with pancreatitis takes about 4 weeks to develop. Abdominal trauma caused by bicycle handle bar, ATV’s, high-speed motor vehicle accidents (seat belt injury) or NAT can lead to pancreatic pseudocyst. Pancreatic (and duodenal) injuries in children are almost always due to abuse.
Typical symptoms of abdominal injury include nausea and vomiting, abdominal pain, and abdominal distention. Abdominal wall bruising is present in 3 out of 4 patients with abdominal trauma. Abdominal exam findings may not be apparent if the presentation is delayed. A rising amylase level and serial exam are helpful and CT scan can describe the extent of pancreatic and associated solid organ injuries.
In the case discussed above there was a wide differential based on his initial symptoms of fall, limp (questionable hip pain) and later development of gastrointestinal symptoms. Septic hip, reactive arthritis, and toxic synovitis were a possibility with his limp and inability to bear weight. Toddler’s fracture, which is a fracture of tibia is not uncommon in the age (1-3 years). Appendicitis with perforation was unlikely due to lack of right lower quadrant tenderness and there were no peritoneal signs. Other intra-abdominal pathology to consider were bowel obstruction, intussusception, and Meckel’s diverticulum.The diagnosis of NAT requires a high index of suspicion. The leading cause of death from NAT is head injury followed by abdominal trauma [1,2]. This family did have some red flags. One of them was the past history of NAT (femur fracture at 4 months age). In this presentation the parents’ story was very consistent; they had consistently sought medical attention and were seen at two different emergency rooms for an evaluation prior to being transferred to our hospital.
Important learning objectives for PEM/EM physicians: As always; a high index of suspicion is required for the diagnosis of NAT.
REFERENCES
1. Injuries caused by child abuse. Ledbetter DJ, Tapper D; Comprehensive Therapy. 1989 Oct;15 (10);9-13
2. Major blunt abdominal trauma due to child abuse. Cooper et al; J Trauma. 1988; 28(10):1483