Your next case looks like it might be more of a psych situation, but you start with a bedside ultrasound to get a better idea of what’s happening.
You try to hide your frustration as your patient yells at you “I have had numerous doctors from lots of places, including your own people, tell me I should come to the emergency department anytime if I need a STAT MRI of my brain!” Surreptitiously, you take in a slow, deep breath, put on your most empathic smile, and explain to the patient that there must have been a miscommunication. You explain to the patient that she should follow up with her primary care physician and her neurologist for her scheduled follow up appointments. Attempts to explain to her that her outpatient plan is appropriate are met with “This is totally ridiculous! This is the worst service I’ve ever encountered.”
As she storms out of the ED with her hospital gown on, you wonder to yourself if this is just going to be one of those shifts. A nice walk down a quiet hallway seems like a great chance to reset, but your intentions are interrupted with high-pitched screaming and security guards escorting a patient to her room.
“Doc, this lady showed up in triage yelling that there is an alien in her abdomen and that we have to get it out. She came with a family member, but he went to go move the car.” Your triage nurse seems beside herself. “There must be a full moon out tonight.”
Your resident follows you cautiously as you walk into the room behind your security guards who are helping the patient gently onto the gurney. She looks you right in the eye and says “There is an alien in me! You have to get it out right now! It is killing me!”
As your nurses hook her up to the monitor, you see that she is hypertensive, tachycardic, a bit tachypneic, but with a normal oxygen saturation. She feels slightly warm, so you ask your team to get a temperature.
“Get this alien out of me! Get it out! Get it out! Get it out!!!!!” You intentionally sit down on the foot of the bed and offer the patient your hand. “Ma’am, I will take care of you. Can you please tell me what you are feeling right now? Are you having any pain?”
“I’m not crazy! There is an alien growing in my stomach and it is making me insane! Just look at me! My hair is falling out. I can’t sleep. I am crapping every hour and the alien is taking over my body!”
You ask your resident to grab the ultrasound machine as you continue to talk and listen attentively to your patient. She continues to wail that her heart is pounding out of her chest and she thinks the alien is multiplying inside of her.
“Can’t we just HAC her with Haldol-Ativan-Congentin?” your nurse whispers in your ear. “Let’s get a better idea of what is going on right now,” you reply. “She’s not an imminent threat to herself or anyone else right now, and I just want to take a good look at a few things on her first.”
You resident wheels in the ultrasound machine and you ask the patient kindly if you can take a look at her with the ultrasound machine. “I hear what you are saying and I want to help you.”
She nods affirmatively and says “Doc, I’m not crazy. You have to believe me. I’ve been to a bunch of other places and they keep telling me there is nothing wrong with me and that I need to see a shrink. I’m not crazy!”
You squeeze her hand reassuringly and begin your point-of-care ultrasound examination of her heart. You see a normal sized heart with great squeeze. There is no pericardial effusion and other than tachycardia, her heart looks grossly normal. You turn your attention to her lungs and note great lung sliding and some normal B-lines on thoracic ultrasound. There is no pleural effusion and no obvious consolidation. You begin scanning her abdomen and note that there is hyperperistaltic bowel, but no intra-abdominal free fluid.
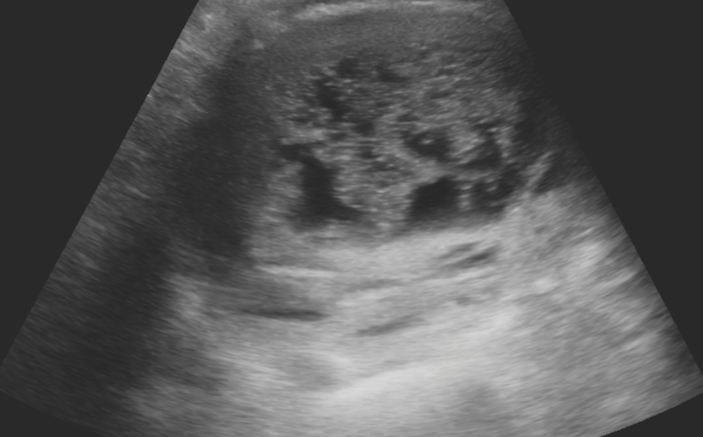
As you scan lower into her abdomen, you obtain the following images:


You continue to scan through the pelvis and capture multiple images of the mass you see growing inside the patient’s pelvis. The mass appears to originate in the pelvis and has mixed, heterogeneous tissue with anechoic areas that suggest a hydatidiform mole with hydropic swelling of trophoblastic villi throughout.
You explain to the patient (and the staff that has gathered around to watch you scan) that you don’t think she is crazy and that you have found the “alien” she has felt growing in her abdomen. You show her the images and videos you obtained on ultrasound and talk her through what you suspect has been going on. You tell her you are going to order a comprehensive pelvic ultrasound through radiology to evaluate her abdominal and pelvic mass further. You also explain that you are going to send some blood tests including a thyroid panel because you suspect she is having signs of thyrotoxicosis from her molar pregnancy. She is so thankful that someone has finally taken her seriously and hugs you with tears streaming down her face. You hear her tell her husband “I told you there was an alien growing inside of me! Now do you believe me?” as you walk out of the room.
As expected, her serum hCG level was over a million mIU/mL. Because hCG resembles TSH structurally, her Free T4 was also extremely elevated, thus accounting for her symptoms and hyperthyroid state. The OB/Gyn team was thrilled to accept your interesting and rare case and helped to schedule an evacuation and curettage of the “alien” in the hospital.
As the patient is being whisked away upstairs for admission, your staff turns to ask you what your secret is for remaining empathic, sympathetic and patient day in and day out in such a strenuous and often stressful field. You smile and note there are many ingredients to the magic sauce, but one of the most important tenets to remember is summarized by Hanlon’s razor “Don’t assume bad intentions over neglect and misunderstanding.” If you remain kind and see people as having good intentions, you will often find that their actions that bother or upset you are only secondary to ignorance or paucity of information.
Armed with Hanlon’s razor, your team is now ready for the rule of threes, the full moon, and Murphy’s Law.
Pearls & Pitfalls For Point-of-Care Ultrasonography
- Point-of-care ultrasound can be used to evaluate and assess a myriad of patient complaints and provide useful data in the assessment of complicated patients.
- Patients with abdominal complaints can be diagnostically challenging because of the various organs that could be causing their symptoms. Use bedside ultrasound to augment your clinical findings and to help expedite care.
- Point-of-care ultrasound can be performed at the patient’s bedside and information can be obtained quickly and accurately without exposing the patient to ionizing radiation.
- Many patients truly enjoy having the physician perform a point-of-care ultrasound because they perceive that the physician is spending more time and engaging in hands-on contact with them during their visit.
- Patients may also enjoy seeing their internal organs on ultrasound, and the images can be used to help educate and teach the patient about their signs, symptoms and diagnoses.
- A transabdominal pelvic ultrasound can be performed with a low frequency transducer to rapidly assess the uterus and adnexa for any large masses, free fluid, or the presence/absence of an intra-uterine pregnancy.
- Remember the diagnosis of a complete or partial hydatidiform mole in your differential when you see a pelvic mass on ultrasound.
- Molar pregnancies are typically described as a heterogeneous mix of tissue from the invasion of the uterus and proliferation of grape-like, swollen chorionic villi. The villi will show up as anechoic or hypoechoic cyst-like circles on ultrasound (bundle of grapes). The old “snowstorm appearance” of molar pregnancies refers to images laden with artifact seen with older, low-resolution ultrasound machines.
- Because the alpha subunit of TSH is nearly identical to that of hCG, some patients with molar pregnancies and extremely high hCG levels will present with signs and symptoms of thyrotoxicosis. Don’t forget this association and think about complications from hyperthyroidism and metastatic trophoblastic disease when evaluating these patients.
- Stay up to date on how you can use bedside ultrasound to enhance your clinical practice and improve patient care with www.SonoSupport.com.

1 Comment
I had a case like this. Patient said they had an alien in their belly, perseverating. I scanned the abdomen – nothing there. They said “thank god!” and we discharged them. Who says ultrasound can’t help with psychiatric issues!