What an interesting week it’s been. You witnessed the untimely death of a young mother and an ED delivery of a newborn in the same shift. You took care of an elderly man with hypermagnesemia and then a young, otherwise healthy man with vomiting and hand cramps that made all his fingers look like they had swan-neck deformities. You just tapped an ankle and diagnosed new onset gout. Now you are about to tap a wrist, and, given how your week has been going, you figure it will probably be pseudogout.
Your wrist pain patient is a 72-year-old man with a history of hypertension and diabetes who presents with three days of progressive right wrist pain, swelling and slight redness. He feels he might have had a slight fever, but didn’t check his temperature at home. He denies any prior joint problems other than some minor arthritis and a torn meniscus in his left knee when he was in college. His review of systems is otherwise unremarkable. On exam, he is afebrile with normal vital signs, and a normal physical exam except for swelling, warmth and faint redness around his right wrist. He has severe pain with active and passive movement of the affected joint. There are no signs of trauma, and his neurovascular status is intact.

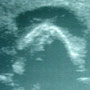
You send off some basic labs and discuss the risk, benefits and alternatives to performing an arthrocentesis. He responds, “What are you going to give me for the pain?” He agrees to undergo the procedure once you promise him that you will address his pain. As the Percocets are kicking in, you explain to your patient that you want to avoid putting him through a painful procedure unless you know for certain that there is an accessible pocket of fluid in his joint. Since wrists are notoriously hard to tap and the procedure is not without risk, you decide to perform a bedside ultrasound to minimize your chances of a dry tap. You obtain the following two images (Figure 1 is of the affected joint, and Figure 2 is of the contralateral side for comparison).

What do you see on your bedside ultrasound? Should you proceed with your arthrocentesis? Conclusion in the following
Dx: Joint Effusion Detected on Bedside Ultrasound

Figure 1 (previous page) demonstrates a moderate sized joint effusion around the distal ulna. The fluid is black and anechoic surrounding the hyperechoic, bright white bony cortex. Note the acoustic shadow farfield to the hyperchoic bone (Figures 3 and 4). Once you see that there is ample fluid to tap, you decide to proceed with the arthrocentesis. You take a few moments to review how to perform the procedure in your favorite pocket ED reference guide, and you scout out an area on his skin that appears clear of any overlying redness or signs of cellulitis. Using ultrasound guidance, you measure how deep the fluid pocket lies, and scan around the area until you find an unobstructed path towards the largest collection of fluid.

**********
Your successful tap reveals positively birefringent crystals, no bacteria, but 74,000 WBC’s per high-powered field. You decide to start treatment for gout. Given his age and risk for co-infection, you and the medicine team decide to admit him for IV antibiotics until his fluid cultures are finalized. Fortunately, his cultures come back negative and the patient is eventually discharged home on hospital day 2 with naproxen and close follow-up.
ARTHROCENTESIS from the Tarascon
Emergency Department Quick Reference Guide


1 Comment
I thought gout had negatively birefringent crystals.