When emergency physician Ken Mwatha fell asleep after a shift, he set in motion a chain of events that would change his life – and his practice of emergency medicine – forever.
When emergency physician Ken Mwatha fell asleep after a shift, he set in motion a chain of events that would change his life – and his practice of emergency medicine – forever.
On March 31, 2010, Dr. Ken Mwatha came home from a long shift as a senior resident at the Johns Hopkins emergency department in Baltimore. Like any other day, he went to the kitchen and began preparing a simple dinner – some chicken wings fried in oil on the stove top. This day, however, something different happened, something that would change Mwatha’s life, and practice, forever. After turning on the burners, Mwatha sat down on the couch in the adjacent living room and fell fast asleep.
The oil in the pan was the first thing to catch fire. The flames leapt quickly to the cupboard next to the stove and within minutes had climbed to the ceiling. It wasn’t long until the entire kitchen was engulfed in flames. Meanwhile, Mwatha lay asleep, just a few feet away, dead to the world in a way all-too-familiar to emergency medicine residents.
With the windows shut, the fire consumed all of the oxygen in the small room. This was both good and bad – the lack of oxygen put the flames out, but turned the small apartment into a literal oven. As Mwatha slept, the room heated to the point that the television began to melt.
The exact movement of the flames through Mwatha’s now-blackened apartment is, of course, conjecture. These facts had to be pieced together by Mwatha and the firemen after the rescue, after they received the 9-1-1 call from a neighbor, broke down his door and dragged his unconscious body from the smoldering room. It was much later that Mwatha learned just how close to death he had come, that he was barely breathing when they arrived.

“I learned a thing or two about non-compliance as I became its poster child,” wrote Mwatha in an account of his experience. After the incident, Mwatha broke down his non-compliant feelings into three parts: territory (the desire to exert one’s free will), ignorance (the feeling of lacking all critical information) and denial (literal disbelief that the injury is real). Through this experience Mwatha has grown more sensitive to patients struggling in these areas.
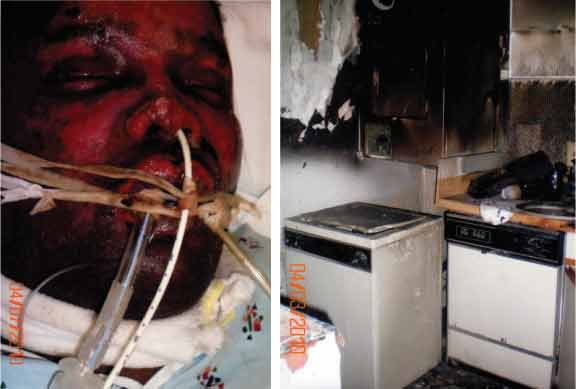
Fortunately, the Sinai Hospital emergency department was only three minutes away. Within minutes of his rescue, Mwatha was brought to the ED, intubated, stabilized and sent off to the Bayview burn center. There they began to address his major inhalation injuries and cutaneous burns. Any part of his skin that had been exposed – his face, arms and feet – was badly burned. In addition, his back, which had absorbed the heat of the couch, also suffered severe burns.
He remained intubated and unconscious for ten days, during which physicians did a graft on his back. They considered grafting his hands as well, which were badly burned, but they knew that this could impact his hand mobility in the future. On the other hand, if they didn’t graft, they knew that it would take much longer to heal. Eventually they chose a wait-and-see approach, a decision Mwatha is still grateful for to this day.
On day ten, Mwatha was extubated.
“That’s the first day I remember,” says Mwatha, who awoke having no idea where he was, or how he had gotten there. Those nearby told him the story, but he had difficulty believing them. His hands were completely bandaged, so he couldn’t immediately see the damage. He didn’t realize he had facial burns until days later when he looked in the mirror. The following day, Mwatha told everyone he felt fine and wanted to go home. That was when they realized that he didn’t understand the extent of his injury, or that he’d been unconscious for 10 days.
Over time, the nurses and Mwatha’s fiancee told him everything that had happened. “I couldn’t fathom it,” he recalls. Finally, Mwatha’s fiancee brought him a photo of his apartment. It finally sunk in; everything was burned.
For two weeks Mwatha battled to recover. At first, anything he tried to drink would go down into his lungs. He couldn’t cough. He was short of breath, even at rest.
“I think the worst part of it was that since I’d been intubated so long, I wasn’t able to swallow and I could only whisper. I couldn’t eat or drink, so I had to be fed through an NG tube.”
It took two weeks before Mwatha was able to walk around the hospital room, all the while he tried to talk his physicians into releasing him.
“Eventually I convinced them to discharge me,” he says. He was still being fed through an NG tube, but his fiancee, a nurse, felt comfortable taking care of this while he began physical therapy from home.
One day during therapy, Mwatha had a chance to view his chart, including the results from a bronchoscopy. He was stunned to see just how black his lungs had gotten. He also read that he’d lost a lot of blood and had received transfusions. Everything started to sink in as he connected his near-death injury with his weeks of weakness and pain.
Eventually, Mwatha returned to the hospital for a swallow study, which he passed, and then gratefully removed the feeding tube. By the third week of May, less than two months after the incident, he was able to return to work.
“I wanted to prove to myself that I could still physically do the job. I wanted to get procedures done. I wanted to do a lot, especially with my hands, because my hands were badly affected . . . it was a relief to realize that I could still do my job.”
*****************
It’s been a few months since the fire. His voice is still a bit raspy due to scarring in his larynx, but Ken Mwatha is back to work. He’s even able to play soccer and exercise. He’s gotten married and he’s moved into a new apartment with his wife. When asked what he’s learned from the ordeal, Ken Mwatha cites a renewed sense of empathy.
“I got a better feel for what it feels like to be a patient,” said Mwatha, who described the “sheer helplessness” that comes with using a beside commode and then having someone come and clean it up. “This is something we do every day at work, but we never think about how humiliating that is, or how vulnerable someone feels in that state.”
“I have a lot more empathy. I’ve realized that people are vulnerable. A lot of patients get angry when we give them a diagnosis. And now I think I understand that anger.”
Mwatha’s own recovery has also made him more cognizant of pain. “I grew up with the mentality that pain is a virtue, and that you suck it up. You’re a man and you don’t whine. But when I was in the hospital, I was in a lot of pain initially. At first, I refused pain medication. I had three or four days of being in a lot of pain. Then I asked myself what I was gaining out of it. At that point I started getting the medication. Now I offer pain medication to my patients up front. I hit ‘em hard and early because I realize now how much suffering can come from pain.”
Mwatha still thinks about the accident every day, about just how close he came to dying. Five more minutes, they tell him. That’s how long until he would have suffocated.
“That blows me away. It blows me away how far I’ve come, from the first few days when I couldn’t lift a cup and couldn’t sit up in bed without being horribly short of breath. And now, I’m going out and playing soccer. I’m not 100% yet, but I’ve come a long way.”
At the end of the day, Mwatha joins the ranks of near-death survivors who have found profound meaning in their
experience. Though he’d never want to relive the horrors of the fire, he can look back now and be thankful for the lessons he’s learned.
“I think I’m better off for everything that happened,” he says. “I really didn’t lose anything that’s not replaceable. I was overwhelmed by the support that I got from the Johns Hopkins community, from friends and family, and everyone else who showed up at my bedside.”

6 Comments
Kitchen safety and gas leak warnings received. Measures taken: always crack windows when using gas stove. Others?
noncompliance?? you have got to be kidding me. i crashed my car once trying to get to weekly conference post-call. this guy’s residency program better have paid for his icu stay.
If there is a fire, I will save myself first and let everyone else, no matter the degree of emotional attachment, young and old alike, perish. No first responder in this scenario. I am not going to feel an obligation towards any fire-fighters or rescuers. What do I have to “forget about” to avoid this?
Yet more evidence that residents are dangerously overworked. The residency program should be tried for this. BTW, my mother (in the 80’s) was rear ended by a fellow resident, post-call; the guy fell asleep at the wheel.
I do think think this stresses the importance of interconnected smoke and heat alarms. A heat alarm in the kitchen (set to go off at 135F) would have detected this before the cabinets ignited and a smoke alarm in the general living area would have detected the subsequent smoke. Though, given the layout of the place, he would have done well with a photovoltaic one as I imagine with his cooking style, an old-school ionization would have had a ton of false alarms.
Anyways it is stories like this that made me finally update the fire alarms in my house to meet the latest residential codes. You really do only have a minute or two to gtfo once a fire like this starts and early warning is important. However, again, while not required, heat alarms are a good idea for kitchens. I’d also throw one in the garage in case the car decides to light itself on fire (aka the ford/GM cruise control incidents).
Wow. I’m so sorry Dr. Mwatha had to learn about the many facets of being a serious patient in that fashion. I’ve seen a lot of medical personnel be totally gobsmacked after their first time on the receiving end, and I’m very glad it’s made him a more mindful doctor. If only there were a way to get those lessons across to everybody without subjecting them to trauma.
Trust me. Hes my dad and i got the message loud and clear. I didnt realize how much patient go through. I nearly broke to tears while looking at my deformed father.