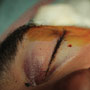
An assault to the face leaves your patient in need of an emergency lateral canthotomy to relieve the pressure and preserve vision. Here is a step-by-step pictorial guide, in case ophthalmology isn’t immediately available.
On a warm summer night, a 35-year-old male is brought in by ambulance after being assaulted fist to face with loss of consciousness. Bystanders witnessed the event. Upon arrival to the ED, he is unresponsive and was intubated prior to arrival for airway protection.
ABC’s are confirmed and ETT is confirmed by direct laryngoscopy. Secondary survey only reveals facial trauma, the patient is otherwise atraumatic. Plans are made for CT scan to evaluate for intracranial trauma. However, there is significant left periorbital ecchymosis and proptosis. The decision is correctly made to quickly assess the globe prior to CT scan. The globe appears proptotic. An afferent pupillary defect is present and tonopen reveals intraocular pressures of 43 in the left eye and 18 in the right eye.
What do we do with this information? Release the pressure by preforming a lateral canthotomy and catholysis. This is an ocular emergency and ophthalmology should be immediately consulted. Unfortunately they are often not available in a timely manner, and this vision saving procedure should be in our bag of tricks.
Background
Orbital compartment syndrome occurs because the globe is in a relatively closed space entrapped between bone and eyelids which are anchored to the orbital rim by the medial and lateral canthal ligaments. In trauma, retrobulbar hemorrhage may force the globe anteriorly causing increased intraocular pressure. Resulting compression of the optic nerve and retinal artery will lead to ischemia and, ultimately, visual loss. Lateral canthotomy and cantholysis will release this pressure and must be performed rapidly once a diagnosis of orbital compartment syndrome is made as the ischemic retina will not regain function.
Physical exam clues
In the responsive patient, loss of visual acuity, diplopia, eye pain and ophthalmoplegia are associated with increased intraocular pressure. However, with the non-responsive patient, rely primarily on physical exam findings such as proptosis, tonopen pressures greater than 40mmHg, afferent pupillary defect, and a blanched optic artery and cherry red macula on fundoscopic exam. The presence of the afferent pupillary defect (APD), also known as a Marcus-Gunn pupil, is evaluated for by the swinging flashlight test. An APD exists when the afferent pathway of the optic nerve is blocked (by trauma, lesions, or ischemia) and no light travels past this lesion to the brain, thus the opposite eye will NOT constrict. To evaluate for APD, shine the light into the affected eye and there will no direct or consensual constriction. However, when light is shined into the non-affected eye, bilateral pupillary constriction still occurs.
Indications
Absolute indications for emergent canthotomy include a retrobulbar hemorrhage resulting in the following:
1. Loss of visual acuity
2. Increased intraocular pressure (greater than 40mmHg in the unresponsive patient)
3. Proptosis
Emergent canthotomy may be considered in the following: ADP, ophthalmoplegia, and severe eye pain. In this situation, a CT scan may be beneficial to evaluate the extent of retrobulbar hemorrhage.
Complications
As with most procedures, bleeding and infection top the list for complications. Due to the proximity of the procedure to the globe, globe rupture is the most concerning complication which can be avoided with assuring all instrumentation is angled away from the eye.
Bedside lateral canthotomy, step-by-step
1. Sterilize the area with betadine.

2. Anesthetize from the lateral fold to the orbital rim using 2cc of lidocaine with epinephrine (a TB syringe or 27 gauge works well). Insert needle into the lateral canthus and inject laterally from the globe. The epinephrine will help provide hemostasis for the procedure.

3. Along this same trajectory, insert hemostats at the lateral palpebral fissure, with one blade anterior to and one blade posterior to the lid. Advance until the orbital rim is encountered and compress the tissue for at least 30 seconds. This will minimize bleeding, but is not an essential step.

4. Use the iris scissors to incise the lateral canthal tendon. Begin the incision at the lateral canthal fold and extend laterally toward the lateral orbital rim cutting the canthal ligament with the iris scissors directed inferoposteriorly away from the globe. Aiming inferoposteriorly toward the lateral orbital rim helps avoid important structures located in the upper lid such as the levator muscle, lacrimal gland, and lacrimal artery.
5. The prior step will release some pressure from the globe; however to fully release the globe a cantholysis must be performed. Pull the lid down to visualize the inferior crus* (if unable to visualize secondarily to bleeding it can be palpated). Direct the iris scissors along the lateral orbital rim (again AWAY from the globe) and cut through the inferior crus to release the globe.
*The lateral canthal tendon divides, like a Y, into a superior and inferior component.

6. Retract the lower lid outward to assure laxity of the lateral canthus and the inferior canthal ligament. Also recheck intraocular pressures to confirm a successful procedure.

References
- Bord SP, Linden J. Trauma to the globe and orbit. Emergency Medicine Clin North Am. Feb 2008;26(1):97-123, vi-vii.
- Lima V, Burt B, Leibovitch I, Prabhakaran V, Goldberg RA, Selva D. Orbital compartment syndrome: the ophthalmic surgical emergency. Surv Ophthalmol. Jul-Aug 2009;54(4): 441-9.
- Carrim ZI, Anderson IW, Kyle PM. Traumatic orbital compartment syndrome: importance of prompt recognition and management. European Journal of Emergency Medicine. Jun 2007;14(3):174-6.
- Goodall KL, Brahma A, Bates A, Leatherbarrow B. Lateral canthotomy and inferior cantholysis:ectiveanmethod of urgent orbital decompression for sight threatening acute retrobulbar haemorrhage. Injury. Sep 1999;30(7):485-90.
- Knoop K, Trott A. Ophthalmologic procedures in the emergency department–Part I: Immediate sight-saving procedures. Acad Emergency Medicine. Jul-Aug 1994;1(4): 408-12.
- Roberts JR, Hedges JR, eds. Clinical Procedures in Emergency Medicine. 5th ed. Portland, Ore: WB Saunders Co; 2009:Chap 63 1174-1177.
Anna Engeln, MD and Brandy Drake MD are 3rd year Emergency Medicine Reside
nts at the Denver Health Emergency Medicine Residency Program. David Richards MD, FACEP and Dr. Peter Pryor are faculty members at Denver Health and Assistant Professors of Emergency Medicine at the University of Colorado School of Medicine. Dr Pryor has an academic focus in medical photography and can be reached at Peter.Pryor@dhha.org.
Leave a comment or pose a question below or on twitter @epmonthly