An 84-year-old woman is brought to the emergency department by ambulance for evaluation of altered mental status and syncope. Per family, the patient had complaints of abdominal pain for two days, tactile fevers, decreased PO intake and one episode of non-bloody, non-bilious vomiting. The patient also fell from her bed to the carpet with loss of consciousness for 10 seconds. Her review of systems is negative for: focal weakness, aphasia, seizures, chest pain, shortness of breath, cough, jaundice, icterus, change in stool color, dysuria, hematuria, urinary odor, diarrhea, hematemesis, hematochezia and melena.
At baseline, the patient lives with her son, but is independent in all activities of daily living, and has no physical or mental deficits. Her past medical history is significant for hypertension and hyperlipidemia, and her only medication is hydrochlorothiazide daily.
Her physical exam reveals an elderly female in no acute respiratory distress. Vital signs are significant for tachycardia to 130 bpm and a low grade fever to 38.3C. Initial blood pressure was normotensive at 114/90 mmHg. Abdominal exam was notable for mild periumbilical tenderness. There were no significant neurological deficits and the patient was alert and oriented x 2. She was noted to have waxing and waning confusion during her ED evaluation. The remainder of the physical exam was unremarkable.
A stat head CT and cervical spine CT without contrast revealed no acute intracranial hemorrhage or relevant findings. Upon returning to the emergency department, the patient was noted to be hypotensive with a blood pressure of 80/40 mmHg which responded to a 1L normal saline bolus. Initial I-STAT laboratory studies demonstrated an elevated Troponin I (0.93), a leukocytosis with a left shift (15.7 with 95% neutrophils) and an EKG with sinus tachycardia and no other acute abnormalities.
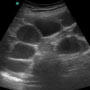
Given the patient’s hemodynamic instability and altered mental status, an emergency bedside ultrasound was performed. Her cardiac exam showed a hyperdynamic left ventricle without wall motion abnormalities or pericardial effusion. The IVC was collapsible. There was no abdominal aortic aneurysm or abdominal/pelvic free fluid. These findings were consistent with a high output, low volume state, which with no evidence of bleeding, was consistent with distributive shock. Given her abdominal tenderness on exam, a RUQ ultrasound was performed to evaluate the hepatobiliary system. This showed a dilated common bile duct with several prominent stones (Figures 1 and 2).


Gastroenterology and general surgery were immediately consulted for evaluation of a patient with choledocholithiasis and septic shock with suspected ascending cholangitis. Broad spectrum antibiotics were initiated to cover an intra-abdominal infection, and further IV fluid resuscitation was provided. The patient’s comprehensive laboratory studies revealed a sodium of 140, chloride of 106, potassium of 2.8, serum bicarbonate of 21, serum urea nitrogen of 28, and creatinine of 1.3. Her total bilirubin was 4.6 and her direct bilirubin was 2.8. Liver function tests showed an AST of 172, ALT of 359, and alkaline phosphatase of 206. Lipase was 14.
The patient had emergent ERCP with stent placement within 6 hours of initial presentation. ERCP showed choledocholithiasis (4 stones, largest 8 mm) with complete obstruction. The patient was admitted to the MICU, continued on antibiotics, extubated on POD #1, and eventually transferred to the medical floor. The patient was discharged home on levofloxacin with full return to baseline functional status on POD #3.

Case Discussion
Cases such as this pose a significant challenge for the emergency physician. An elderly patient with altered mental status, vague abdominal complaints, a recent fall with syncope, and an elevated troponin, has many different possible etiologies. Initially, our main concerns were intracranial hemorrhage, stroke, MI, AAA, GI bleed, sepsis, ingestion, electrolyte disturbance, and obstruction. The patient became hypotensive after returning from her CT scans and was unstable for further transport outside of the department. Emergency bedside ultrasonography was instrumental in making a prompt diagnosis, which allowed for immediate treatment and a favorable outcome.
The CORE scan (Concentrated Overview of Resuscitative Efforts) and the RUSH protocol (Rapid Ultrasound for Shock and Hypotension) are two common ultrasound algorithms that should be used during the assessment and management of patients who present with shock1,2. Ultrasound can provide valuable information to differentiate between distributive, cardiogenic, and obstructive shock within minutes at the bedside. Furthermore, bedside ultrasound can be used to assess for life-threatening etiologies that require immediate intervention. While the patient is being evaluated, bedside ultrasound can help guide resuscitative options and determine if the patient is responding appropriately to interventions.
In our patient, the hyperdynamic LV and collapsible IVC were consistent with high output/low volume state. This made cardiogenic shock (which usually shows a hypodynamic LV, wall motion abnormalities, and distended veins) less likely despite her elevated troponin. Thus, we were able to liberally bolus the patient with IVF’s rather than consider inotropic therapy and possible cardiac catheterization. The normal diameter of the aorta and the lack of intraperitoneal free fluid, together with lack of obvious bleeding and a guaiac negative rectal exam, helped to rule out hypovolemic shock. We were thus able to make the diagnosis of septic shock and treat the patient quickly and appropriately with fluid resuscitation and antibiotics. Our bedside ultrasound evaluation of the patient helped us make this diagnosis, guide treatment, and avoid unnecessary workup which would have delayed necessary interventions.
Once the diagnosis of sepsis is made and goal directed therapy is initiated, the next priority is source identification and control2. Emergency bedside ultrasonography can quickly assess for etiologies that may otherwise require time-intensive imaging outside of the emergency department. In our case, bedside ultrasonography allowed us to visualize CBD stones and dilation, and make the diagnosis of cholangitis within minutes. This was possible despite lack of typical symptoms like jaundice and RUQ tenderness4.
There is no literature specifically investigating the competency of emergency physicians in detecting choledolcholithiasis with bedside ultrasound, but there is evidence supporting their competency in detecting stones and inflammatory changes in the RUQ with this modality. According to a study published in the Journal of Emergency Medicine in 2001, Emergency Physicians were able to detect gallstones by bedside ultrasonography with a sensitivity of 96%. They were able to detect a sonographic Murphy’s sign and acute cholecystitis more frequently than formal ultrasounds (EP sensitivity 75% vs. formal ultrasound sensitivity 45%). Furthermore, most EPs (83%) completed the studies in under 10 minutes5.
Another study published in the Annals of Emergency Medicine in 2010 compared the accuracy of emergency physicians at detecting cholecystitis with bedside ultrasound to that of radiology ultrasonography and found them to be comparable. EPs assessed for cholelithiasis, sonographic Murphy’s sign, gallbladder wall thickness, and pericholecystic fluid. The sensitivity of EPs was 87% (CI 66-97), specificity 82%. The sensitivity of formal radiology ultrasound was similar, at 83% (CI 61-95), specificity 86%6. Although further studies are needed, it appears that EPs have a comparable level of competency to radiologists at RUQ ultrasounds. This competency will continue to improve as bedside ultrasound becomes a greater part of residency training and the practice of emergency medicine, especially in the critically ill.
Increased utilization of bedside ultrasonography will lead to faster diagnosis and treatment, and consequently better outcomes, as it did in the case of this patient with septic shock from cholangitis.
Tips & tricks for the RUSH and CORE scans
1. Perform the RUSH or CORE scans to aid in rapidly identifying the etiology of a patient’s hypotension. These should be performed in conjunction with and not in place of other diagnostic modalities (labs, EKG, etc.)7
2. Look at the pump (heart) first with the goal of answering three primary questions. Is there a pericardial effusion or tamponade? Is LV contractility decreased? Does the RV appear large compared to the LV? If the answer is yes, consider cardiac tamponade, cardiogenic shock, or massive pulmonary embolus, respectively. The apical 4 chamber or subxiphoid views may be adequate to obtain this information though additional views can be required.
3. Look next at the tank (volume status). Look at the IVC for respiratory variability and also at the lungs and abdomen (FAST). IVC collapsibility suggests volume depletion while pleural or peritoneal fluid may indicate why the patient is volume depleted.
4. To save time, after obtaining the RUQ and LUQ views of the FAST exam, slide the transducer in the cranial direction to evaluate the thorax for pleural effusion, pneumonia, pneumothorax, etc.
5. Finally look at the pipes (large veins/arteries). Examine the abdominal aorta for signs of aneurysmal dilatation and the femoral and popliteal veins for non-compressibility suggestive of DVT and therefore possible PE.
6. When evaluating for pneumothorax, remember that a right mainstem intubation or bronchial obstruction may mimic the sonographic appearance of pneumothorax (absent lung sliding) just as they can mimic the physical exam findings of pneumothorax (absent breath sounds) 7. The CORE scan will teach you how to identify the sonographic differences between a left sided pneumothorax and a right mainstem intubation.
7. The mnemonic HI-MAP (Heart, IVC, Morrisons/Fast, Aorta, Pneumothorax) can help you remember the most basic components of the RUSH/CORE exams. Additional scans can be performed as clinically indicated. In this case, the patient was complaining of abdominal pain which prompted further evaluation of the biliary system and led to rapid identification of the likely etiology of this patient’s hypotension.
8. Though the exam can be performed in less than two minutes in the hands of a skilled sonographer, take your time and be deliberate as it is easy to miss or misinterpret important findings. A pitfall of the exam is to scan too quickly and miss a key finding 7.
References
(1) Wu, Teresa. The CORE Scan: Concentrated Overview of Resuscitative Efforts. Critical Care Clinics. January, 2014. EPub Ahead of Print.
(2) Perrera, Phillips, et al. The RUSH Exam: Rapid Ultrasound in Shock in the Evaluation of the Critically Ill. Emerg Med Clin North Am. 2010 Feb;28(1):29-56, vii.
(3) Dellinger, Phillip, et al. Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008. Intensive Care Med. 2010 Feb;36(2):222-31. Epub 2010 Jan 13.
(4) Rosh, Adam, et al. Cholangitis in Emergency Medicine. Last update 6/11/2010. http://emedicine.medscape.com/article/774245-overview.
(5) Kendall JL, Shimp RJ. Performance and interpretation of focused right upper quadrant ultrasound by emergency physicians. J Emerg Med. 2001; 21(1): 7-13 (ISSN 0736 – 4679).
(6) Summers SM, et al. A prospective evaluation of emergency department bedside ultrasonography for detection of acute cholecystitis. Ann Emerg Med. 2010; 56: 114-22 (ISSN 1097 – 6760)
(7)”RUSH.” Mount Sinai Emergency Medicine Ultrasound. N.p., n.d. Web. 05 Dec. 2013..