A 28-year-old male presents to the emergency department with a chief complaint of chest pain, coughing and shortness of breath. After being discharged with normal x-ray results, he winds up returning to the ED with the same symptoms. Find out the culprit and the best practices to manage the diagnosis.

A 28-year-old male presents to the emergency department with a chief complaint of chest pain, coughing and shortness of breath. He reports that about seven hours prior to presentation he was having a dental procedure and that he may have swallowed some gauze.
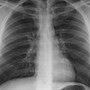
He is taken from the dental clinic to radiology where a chest x-ray [pictured]is obtained and read as normal. The patient is discharged, but a day later develops a cough for which he takes Nyquil. He also develops worsening shortness of breath aggravated when lying down and taking deep breaths. He denies any fever or hemoptysis.
His past medical history is significant for peptic ulcer disease with hematemesis. He does not routinely take any medications and does not have any allergies. He smokes about one pack of cigarettes daily and uses alcohol recreationally. On physical examination he appears alert, slightly anxious and mildly dyspneic. His pupils are equal and reactive and his oropharynx is clear. Heart is regular rate and rhythm. His lung exam demonstrates diffuse wheezing more on the left than the right without rhonchi or rales. Chest rise is symmetric.
The chest x-ray done earlier is reviewed and shows no acute abnormality. Given the progression of his symptoms a CT scan of the chest is obtained.
Click here for case conclusion
The CT scan showed a foreign object within the distal left mainstem bronchus consistent with the gauze or a portion of a tooth (Figures 2-3). The remainder the examination was within normal limits. Pulmonology was consulted and the patient was taken to bronchoscopy for removal of the foreign body which was subsequently identified as a piece of surgical gauze.

Figure 1: Chest CT (axial view) demonstrating foreign body

Figure 3: Chest CT (coronal view) demonstrating foreign body
Discussion
Aspiration or ingestion of foreign bodies during dental procedures is an infrequent but well reported complication of dental and oral surgical care.[1,2] These events most commonly occur during the placement of crowns, extraction of teeth, and procedures surrounding dental prosthetics.[1,2,3] The complications of ingestion and aspiration are potentially life threatening and include airway obstruction, esophageal impaction, viscus perforation, pneumonia, lung abscess, and post-obstructive pneumonitis.[2,3]
While aspiration is less common than ingestion, the complications of aspiration are generally more immediate and carry a higher morbidity and mortality.[4,5]
Patients experiencing aspiration during a procedure will often have a brief period of intense coughing. This may be followed by clinically evident obstruction or partial obstruction, protracted coughing without obstruction or an asymptomatic period. In addition to cough, which is the most common presenting symptom, patients may present with fever, chest pain, hemoptysis and dyspnea following aspiration.[6]
Following basic airway management the initial evaluation of a patient with suspected aspiration should include evaluation of the oropharynx and lungs. A chest x-ray and abdominal film should be obtained to look for a radiopaque foreign body, free air and signs of post-obstructive air trapping.[7] Foreign bodies are most prone to lodge in the right main stem bronchus due to its larger diameter and more vertical orientation compared to the left main stem however, this patient had a left main stem aspiration.[6] In patients where aspiration is still suspected and symptoms are minimal, CT scan is a useful next step. In one study 100% of tracheobronchial foreign bodies were identified with CT.[7] For patients with identified tracheobronchial foreign bodies consultation with specialists skilled in bronchoscopy should be obtained immediately. Patients with negative imaging but ongoing symptoms or very high suspicion of aspiration should be evaluated for urgent bronchoscopy.
Patients with symptoms suggestive of acute or subacute aspiration following dental or oral surgery procedures should be evaluated appropriately on presentation to the ED. Since these events are relatively uncommon and patients may not make the association between the procedure and onset of symptoms emergency physicians must maintain a high index of suspicion for foreign body aspiration and perform appropriate history and evaluation of these patients.
REFERENCES
1. Tiwana K, Morton T and Tiwana P. Aspiration and ingestion in dental prac- tice: A 10-year institution review. JADA, 2004;135:1287-1291.
2. Obinata K ,Satoh T, Towfik A and Nakamura M. An investigation of accidental inges- tion during dental procedures. J Oral Sci, 2011;53(4):495-500.
3. Medical Emergencies in the Dental Setting. Http://www.netce.com/coursecontent. php?courseid=708. Accessed March 7, 2012.
4. Cevik M, Gokdemr MT, Boleken ME, et al. The characteristics and outcomes of foreign body ingestion and aspiration in children due to lodged foreign body in the aerodigestive tract. Pediatr Emerg Care. 2013;29(1):53-7.
5. Shah R, Patel A, Lander L, Choi S. Man- agement of foreign bodies obstructing the airway in children. Arch Otolaryngol Head Neck Surg. 2020;136(4):373-379.
6. Mahmoud M, Imam S, Patel H, and King M. Foreign body aspiration of a dental bridge in the left main stem bronchus. Case Re- ports in Medicine. 2012, Article ID 798163.
7. Bai W, Zhou X, Shao C, et al. Value of chest CT in the diagnosis and management of tracheobronchial foreign bodies. Pediatrics International, 2011;53:515-518.