A 43-year-old diabetic male presented to the emergency department with a complaint of right eye irritation for one day. He reported that the day prior he was sanding fiberglass and, when he finished, he had a foreign body sensation in his right eye.
A 43-year-old diabetic male presented to the emergency department with a complaint of right eye irritation for one day. He reported that the day prior he was sanding fiberglass and, when he finished, he had a foreign body sensation in his right eye.
Presentations can vary, but urgent diagnosis is always essential

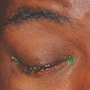
Image 1: Initial Presentation
A 43-year-old diabetic African-American male presented to the emergency department with a complaint of right eye irritation for one day. He reported that the day prior he was sanding fiberglass and, when he finished, he had a foreign body sensation in his right eye for which he irrigated his eye with an eye solution. He awoke the morning of initial presentation with a mild crusting and a drooping upper eyelid. He also reported intermittent double vision. He denied headache, light sensitivity, purulent eye discharge, or other neurologic complaints. He does not wear contact or corrective lenses. He reported wearing eye protection while working. His past medical history was notable for hyper-tension and diabetes.
On initial examination, his visual acuity was 20/30 bilaterally. A mild ptosis versus upper eyelid edema was noted. There was no chemosis or proptosis but mild conjunctival injection was present. Anisocoria of 1-mm was appreciated (the right pupil was larger); however, both pupils were reactive to light. Extraocular muscles were intact without re-producible diplopia. Fluorescein exam was negative for corneal abrasions and there was no noted cell or flare in the anterior chamber. The rest of his neurologic exam was normal. The EP concluded the patient had eye and eyelid irritation from fiberglass; he was given artificial tears, and instructed to follow-up with ophthalmology the following day.
Throughout the evening, the patient had progression of his symptoms with constant diplopia and photophobia. At a follow-up visit with ophthalmology the following morning, he had stable visual acuity. Prominent ptosis was now present. Pupillary exam demonstrated a mid-dilated, poorly reactive pupil and marked restriction of extraocular eye movement in all directions except for lateral gaze in the right eye with a “down and out” resting state. (figures 1-4). Due to the concern for a 3rd nerve/cranial nerve palsy with pupil involvement, the patient was transferred urgently to the emergency department to undergo neuroimaging to exclude aneurysmal compression of the cranial nerve. The patient underwent unremarkable CT angiography with no aneurysm or intracranial etiology found. He was subsequently diagnosed with microvascular diabetic 3rd nerve palsy. The temporal relation of the onset of symptoms to sanding fiberglass was a coincidental red herring.

Image 2: Left Lateral Gaze

Image 3: Right Lateral Gaze

Image 4: Upward Gaze
Discussion: 3rd Nerve Palsy
Cranial nerve III (oculomotor nerve) originates as a cluster of nuclei in the midbrain at the level of the superior colliculus and exits the midbrain ventrally, travelling through the subarachnoid space in the interpeduncular cistern. In the subarachnoid space it passes the basilar artery, superior cerebellar artery, and most importantly, adjacent to the posterior communicating artery of the Circle of Willis. The nerve then enters and travels along the lateral wall of the cavernous sinus with cranial nerves IV, V, and VI as well as the carotid artery where the nerve divides into a superior and inferior branch. It terminates to innervate the levator palpebrae superioris as well as four of the six extraocular muscles: the superior rectus, inferior rectus, medial rectus, and inferior oblique muscles. It also carries parasympathetic innervation from the ciliary ganglion to the constrictor pupillae and ciliary muscles external to the nerve along its superficial periphery. The levator palpebrae superioris elevates the upper eyelid. The innervated extraocular muscles control all eye movements with the exception of abduction (cranial nerve VI/abducens nerve) and inferior-medial gaze (cranial nerve IV/trochlear nerve). The parasympathetic innervation causes pupillary constriction and accommodation.
Clinical Presentation
The clinical presentation of a 3rd nerve palsy can be markedly varied depending on whether the palsy is complete or incomplete and whether or not it is pupil-sparing or pupil-involving. Patients may complain of a headache/eye pain, drooping eyelid, light sensitivity, blurry vision or double vision. Based on the completeness of the palsy, physical exam may demonstrate varying ptosis, an inferiorly-laterally deviated or “down and out” pupil at resting gaze due to the unopposed actions of the lateral rectus and superior oblique muscles. Extraocular muscle exam may demonstrate difficulty with superior and medial gaze. If there is pupillary involvement, the pupil will be dilated compared to the unaffected eye.
The pupil may be poorly reactive/non-reactive and lack accommodation due to loss of the parasympathetic innervation of the pupil. Central causes of 3rd nerve palsy typically have other neurologic exam findings.
Pathophysiology
Dysfunction of cranial nerve III can result from lesions anywhere along its path from its origination at the oculomotor nucleus in the midbrain to the extraocular muscles within the orbits. Brainstem lesions are typically neurologically non-isolated, and frequently have associated bilateral ptosis, contralateral ataxia and/or weakness. Lesions within the cavernous sinus or orbit usually demonstrates other cranial nerve palsies such as IV, V, VI as well signs of venous congestion including chemosis or proptosis. Isolated cranial nerve III lesions can be pupil-involving or pupil sparing. Ischemic etiologies (e.g., hypertension, diabetes) are typically pupil-sparing, affecting the microvasculature blood supply deep within the nerve. Pupil-involving cranial nerve III palsies should raise high suspicion for an external compressive lesion to the superficial periphery of the nerve where the parasympathetic fibers reside.
This is commonly called the “rule of the pupil.” The location of cranial nerve III within the subarachnoid space adjacent to the posterior communicating artery should give high clinical concern for a rapid expanding aneurysm of this artery. An aneurysm causing acute 3rd nerve palsy is potentially at eminent risk for rupture and should be rapidly evaluated with neuroimaging.
Treatment
Rapid diagnosis of concerning pupil-involving 3rd nerve palsies is of utmost importance due to risk of aneurysmal rupture. MRI/MRA may be considered as it provides evaluation of the neurovasculature as well as may provide clues to other etiologies such as mass lesions, meningitis, vasculitis, etc. CT/CTA is also readily available to the emergency physician and is frequently obtained.
Those with histories concerning for subarachnoid hemorrhage should be considered for lumbar puncture after neuroimaging. High risk patients with normal neuroimaging should have a neurosurgical consult and advanced diagnostic techniques such as cerebral angiogram may be considered. Found aneurysms are treated traditionally with coiling or clipping. Low risk patients over the age of 50 with risk factors for ischemic etiologies such as hypertension and diabetes with pupil-sparing 3rd nerve palsies can be safely discharged with primary care and ophthalmologic follow-up. Vascular risk factors should be appropriately treated. Patching of one eye can alleviate the diplopia in the short term. Prisms may be used to improve alignment of the visual axis. In most cases, diplopia and ptosis recover in several weeks to months. Deficits still present at six months are usually persistent, and may require surgical intervention to alleviate strabismus/diplopia and ptosis.
Chris Wyatt, MD is an attending physician in the Department of Emergency Medicine at MetroHealth Medical Center and an Assistant Professor of Emergency Medicine at CWRU School of Medicine, Cleveland,Ohio.
David Effron, MD is Assistant Professor of Emergency Medicine at Case Western Reserve University and attending physician in the department of emergency medicine at MetroHealth Medical Center.
REFERENCES
1. Biousse V, Newman NJ. Third nerve palsies. Semin Neurol. 2000;20:55-74.
2. Jacobson DM, McCanna TD, Layde PM. Risk factors for ischemic ocular motor nerve palsies. Arch Ophthalmol. 1994;112:961-966.
3. Lee AG, Hayman LA, Brazis PW. The evaluation of isolated third nerve palsy re-visited: an update on the evolving role of magnetic resonance, computed tomography, and catheter angiography. Surv Ophthalmol. 2002;47:137-157
4. Woodruff MM, Edlow JA. Evaluation of third nerve palsy in the emergency department. J Emerg Med. 2008; 35(3): 239-246