Why does it always feel like a battle between good and evil? You want to admit the 78-year-old male who had a syncopal event, but the internal medicine service feels that he can be worked up as an outpatient. You call your vascular surgeon early about a patient with a cold, ischemic foot, and he yells at you for calling before the ABIs and arteriography have been performed. And now, you are arguing over the phone with the OB/Gyn attending who refuses to come down to see a vag-bleeder with a hemoglobin of 6 who is soaking through a pad per hour and feeling faint. “I’ve seen worse…” she spouts out, as if that’s supposed to make you feel less concerned about the poor woman in front of you.
Just then, your charge nurse walks in to tell you that you have a sick trauma patient en route to your ED. In 10 minutes you’ll get a 49-year-old female who broke her femur while riding her bicycle. She was hit by a vehicle in the intersection and thrown off her bike. She’s hypotensive and tachycardic, but otherwise alert and without any other signs of trauma.
On arrival to your trauma bay, she appears rather pale and diaphoretic. She is screaming at the top of her lungs about her broken leg, and you realize this isn’t going to be the peaceful, straightforward case you were hoping to end your night with. Her initial vital signs demonstrate a blood pressure of 82/46 mmHg and a heart rate of 114 bpm. She’s tachypneic, but her oxygen saturation and temperature are within normal limits. Her primary and secondary survey are only remarkable for an obvious closed right femur fracture and some minor abrasions over both legs. You notice that she has a port on her chest, and discover that she has a history of breast cancer, currently being treated with chemotherapy and radiation.
During her resuscitation, she has a normal chest X-ray and a normal pelvis X-ray, and has already received 2 liters of normal saline wide open. Her abdomen remains soft and non-tender, and there are no other signs of trauma other than her right femur. It’s clear by her clinical presentation that your patient doesn’t have much reserve at baseline, and may not do too well with this injury.
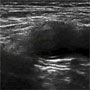
She lies there in front of you screaming for dilaudid and fentanyl, but the trauma team is reticent to give her any IV narcotics secondary to her ongoing hypotension despite treatment with IV fluids. As the O-negative blood is being retrieved to begin a transfusion, you finish up your eFAST exam on the patient and decide to take a peek at the patient’s proximal thigh. You change over to the linear array transducer and obtain the following images.


What do you see? What can you do to help your poor patient? Conclusion in the following

Dx: Managing the Femoral Nerve Block
On your ultrasound image, you have a clear view of the femoral vein medially, femoral artery just lateral to the vein, and a nice shot of the femoral nerve coursing just laterally to the femoral artery (Fig 3). You know it’s going to be tricky managing this patient’s pain given her hypotension and the severity of her injury. Any attempt at reducing her femur fracture or putting it into traction is going to be met with obscenities and further screaming. It would be cruel and unusual punishment to try to reduce this woman’s leg without any analgesia, and she is not an ideal candidate for sedation alone. On the ultrasound image, the femoral nerve is just screaming to be blocked, so you work on attempting an ultrasound guided fascia iliaca compartment block to help treat your patient’s pain.

With your probe resting just below the inguinal ligament, you find the femoral nerve, the femoral artery, and femoral nerve you are very familiar with from femoral venous access attempts. You can visualize the fascia lata, fascia iliaca, and iliopsoas muscle surrounding your femoral nerve and adjacent vessels (Figure 4). You note that the femoral nerve has branches above and below the fascia iliaca. You insert a long spinal needle under your probe and guide the tip towards the area just beneath the fascia iliaca surrounding the iliopsoas muscle. With anesthetic injected into this space, you are able to anesthetize the lateral femoral cutaneous nerve, the femoral nerve, and the obturator nerve.

Now that you see that your needle is in the right place under ultrasound guidance, you aspirate first to ensure you are not in a vessel, and then administer 40 mL of a lidocaine-bupivicaine mixture into the potential space. Within minutes, the patient’s demeanor becomes more calm and collected. Her pain is improving and she can now tolerate a quick reduction and traction applied to her right femur fracture. She thanks you and your team for all of your help, and promises to be a more understanding consultant the next time she is in your ED.
At that last comment, you turn to your trauma colleague with a puzzled look on your face. To which he replies “Yep, that’s the OB/Gyn attending you called to come evaluate your heavy vaginal bleeder in room 9.”
Tips & Tricks for Ultrasound-Guided Fascia Iliaca Compartment Block
01 Secure a longer medium-gauge needle (e.g. an 18 gauge lumbar puncture needle to perform the procedure).
02 Use the 13-10MHz linear array transducer to map out the important anatomical structures. In larger patients, you may need to use the 5-3MHz curvilinear array transducer. Try to directly visualize the femoral artery, femoral vein, femoral nerve bundle, iliospsoas muscle, fascia iliaca, and fascia lata.
03 Scan with your probe resting in a transverse fashion just below the patient’s inguinal crease on the affected side.
04 Remember the mnemonic NAVEL. From lateral to medial, you should see the Nerve, Artery, Vein, an Empty Space, and then the Lymphatic channels.
05 Arteries will appear as thick-walled, round, pulsatile anechoic vascular structures. Veins will have more of an oval shape to them and have thinner walls. Nerves will appear as hypoechoic fascicles embedded within a more hyperechoic perineurium and endoneurium. When nerves are grouped together and viewed in a transverse plane, they appear as “honeycombs”. Distal nerves that are innervating smaller sites may have smaller amounts of myelinated axons, and therefore can be mistaken as tendons. When in doubt, trace the course of the target structure to determine its origin.
06 Nerve blocks should not be used in pat
ients who have an allergy to anesthetic agents, in those with active infection at the site of injection, in patients who are at risk for compartment syndrome, in uncooperative patients who won’t tolerate the procedure, in those with a pre-existing neurological deficit, and in those with are extremely obese thereby precluding adequate visualization of the important target structures. Note that anticoagulation use is a relative contraindication.
07 Once you have found your landmarks and tissue planes under ultrasound guidance, make sure you are looking at the fascia iliacus. The Sartorius muscle crosses the iliopsoas just after it passes over the edge of the ileum and can confuse the picture. Use your probe to find the bright white ilium bone. The muscle lying in contact with the bone and directly overlying it is the iliacus muscle, and the fascial layer above it is the iliacus fascia.
08 Pull up 40-50 mL of your anesthetic of choice. Insert your needle in plane with the ultrasound transducer and aim towards the area just below the fascia iliacus. You will feel two pops. The first pop will be felt as you penetrate through the fascia lata. You will feel a second pop after you poke through the fascia iliaca. Once your needle is inserted underneath the fascia iliacus, inject 40-50 mL’s of anesthetic in a superomedial angle towards the edge of the ileum to bathe all of the nerve fibers traversing downwards to the femoral nerve.
09 Monitor the spread of the muscle fibers and nerve bundles as the anesthetic is instilled. If you are running into resistance during the anesthetic injection, redirect the needle so that it is not aimed directly into any muscle bellies.
10 Pain relief should peak by 20-30 minutes after the injection.
Brady Pregerson manages a free on-line EM Ultrasound Image Library and is the editor of the Emergency Medicine Pocketbook series. For more information visit EMresource.ORG.
Teresa S. Wu is the Associate Residency Director, and Director of Ultrasound and Simulation Programs and Fellowships, for the Maricopa Emergency Medicine Program in Phoenix, Arizona.