Your dejected resident walks away from the patient’s bed to peek at the portable chest X-ray that was just taken.
“I can’t believe I missed that airway!” she says. “I haven’t had that happen in years!” You reiterate how difficult the airway was, and you compliment her on changing her approach between attempts.
“You know, Richard Branson once said, ‘Opportunities are like buses…there’s always another one coming’,” you say. “Why don’t you go see what the EMS call is all about?” Sure enough, the local flight crew is bringing in a 52-year-old male in respiratory distress. He is tachypneic and tachycardic and they are having a hard time getting a history from him. He was initially hypotensive, but his blood pressure has responded well to the liter of normal saline that they just infused. You have five minutes to get everything prepared.
In gearing up for a potentially tricky resuscitation, your once dejected resident is now full of energy. She organizes the troops, assigns roles, double checks all of her airway equipment, and prepares the ultrasound machine. The patient arrives a few minutes later and requires intubation. Like a pro, your superstar senior slides an 8.0 mm endotracheal tube gently through the vocal cords. As the RT’s hook the patient up to capnography, your resident attempts to auscultate for bilateral breath sounds.
“Something’s not right here,” she says. “I can’t hear any breath sounds on the left. I can’t even hear his heart sounds on that side.” Before you can even open your mouth to make the suggestion, she reaches for the ultrasound probe and begins scanning the patient’s chest.
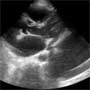
With the phased array transducer, your resident takes a quick look at the patient’s heart in the parasternal long axis (Figure 1). She throws a quick smile your way, and says, “Looks like he’s going to need another procedure.” She obtains a few more views to confirm her findings and scurries off to grab the requisite supplies.
Figure 1: Parasternal long axis view of the heart (click on image to enlarge)
 What do you see on the parasternal long axis view of the heart? What procedure does this patient need?
What do you see on the parasternal long axis view of the heart? What procedure does this patient need?
Dx: Large Pleural Effusion
Your resident comes back into the room with a chest tube tray and Pleurovac in hand. On the parasternal long axis view of the heart you see a large collection of anechoic fluid near the heart. Because it is lying behind the descending aorta, you know that the fluid is in the patient’s lung and not around his heart (Figure 2).
Figure 2: RV = Right Ventricle, LA = Left Atrium,
Asc Aorta = Ascending Aorta, Ao = Descending Aorta (click on image to enlarge)
 You help your resident prep the ultrasound machine so she can perform the procedure in a sterile fashion under dynamic ultrasound guidance. With your probe at T7 in the mid-axillary line, you and your resident visualize a large anechoic left pleural effusion above the diaphragm, cephalad to the spleen. You point out the hyperechoic visceral pleura floating in the pleural effusion so that your resident can avoid the lung parenchyma as she inserts the chest tube under ultrasound guidance (Figure 3).
You help your resident prep the ultrasound machine so she can perform the procedure in a sterile fashion under dynamic ultrasound guidance. With your probe at T7 in the mid-axillary line, you and your resident visualize a large anechoic left pleural effusion above the diaphragm, cephalad to the spleen. You point out the hyperechoic visceral pleura floating in the pleural effusion so that your resident can avoid the lung parenchyma as she inserts the chest tube under ultrasound guidance (Figure 3).
Figure 3: Lung parenchyma floating in a large pleural effusion
 Your resident successfully drains a liter of pleural fluid from the patient’s thorax and his blood pressure begins to improve. You put in an order for a delayed second chest X-ray to evaluate for re-expansion pulmonary edema and you pat your resident on the back for a job well done. With her newfound confidence and the trusty ultrasound machine in tow, she heads out toward the chart rack to see what other opportunities lie ahead.
Your resident successfully drains a liter of pleural fluid from the patient’s thorax and his blood pressure begins to improve. You put in an order for a delayed second chest X-ray to evaluate for re-expansion pulmonary edema and you pat your resident on the back for a job well done. With her newfound confidence and the trusty ultrasound machine in tow, she heads out toward the chart rack to see what other opportunities lie ahead.
Editor’s Notes
1. Diagnostic ultrasound is 93% sensitive for pleural effusion (Lichenstein 2009) and sonographic evaluation of non-traumatic pleural effusions can change emergency physician treatment plans in 43% of cases (Tayal 2006)
2. Among other etiologies, pleural effusions can result from CHF, PE, ARDS, or pneumonia, and sonography can help distinguish each of these diagnoses (Volpicelli 2008, Copetti 2008) so don’t just focus on the effusion.
3. Ultrasound may someday play a role in timely out-of-hospital decision making by improving diagnostic accuracy (Lapostolle 2006).
4. Sonographic procedural guidance can enhance patient-safety in the hectic ED by reducing “wrong-sidedness” (Shapiro 2003) and by reducing iatrogenic pneumothorax (Feller-Kopman 2007)
5. Employing ultrasound in emergency practice can yield positive return-on-investment (i.e. become financially rewarding) within 5-years (Soremekun 2009).
Search Strategies
Want to keep up with the literature on diagnostic
ultrasonography for free? Follow these easy steps:
a) Go to PUBMED: http://www.ncbi.nlm.nih.gov/pubmed
b) Select “Clinical Queries” (at the bottom under PUBMED tools) and then diagnosis broad/sensitive before entering a search for “pleural effusion”
c) Conduct another two searches: “ultrasonography” and “emergency”
d) Combine the clinical query search with the ultrasonography and emergency searches.
e) You can save your search to re-run periodically by signing up for an account on “My NCBI” http://www.ncbi.nlm.nih.gov/sites/myncbi
Don’t miss this feature ultrasound video
Differentiating Pleural and Pericardial Effusions on Ultrasound