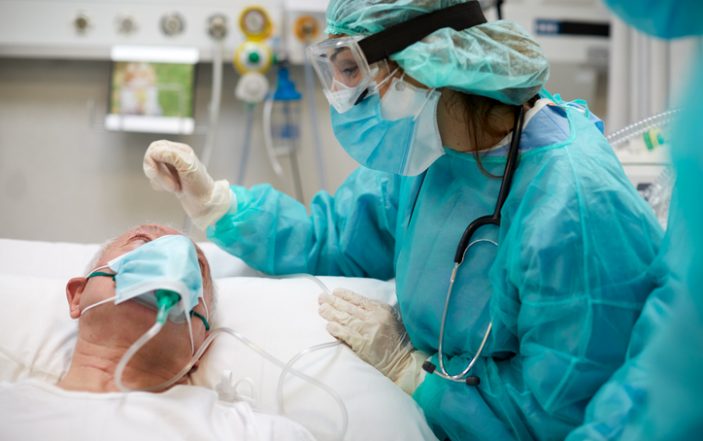
Hyperbaric Oxygen Therapy is emerging as a new strategy for severe COVID-19.
A second US-based clinical study (Gorenstein et al.) again demonstrated the safety of utilizing Hyperbaric Oxygen Therapy (HBOT) in patients with significant acute respiratory effects of COVID-19.[1] Several of this study’s authors were emergency physicians.
In both of the current US-based studies (Gorenstein eet al.; Thibodeaux et al.,) study participants were patients admitted with confirmed COVID-19 diagnosis. They were developing worsening respiratory symptoms, thus facing the possibility of intubation/ventilation and/or increased morbidity/mortality. [1,2]
Patient candidates for both studies were initially identified by the patient’s clinical providers as having increasing respiratory needs. In the Thibodeaux study, five patients were identified and received up to six (daily) HBOT interventions.
Though their providers identified these patients as progressing toward intubation/ventilation, none subsequently required intubation/ventilation and improved during and after HBOT. In the Gorenstein propensity-matched control study, 20 patients received up to five daily HBOT interventions compared with 60 controls who received standard of care. HBOT-treated patients demonstrated improvement as compared to controls with reduced mortality (10% vs. 22%) and improvements in time to discharge home (90% vs. 73%).
The Thibodeaux study was a retrospective report of patients clinically treated with HBOT as “off label” therapy. The Gorenstein study was performed as a clinical trial effort prospectively approved by the site’s IRB and registered with clinicaltrials.gov. While neither of these efforts is a prospective, randomized control trial and both have low numbers of HBOT-treated patients (n=5, n=20), both have confirmed the safety of utilizing HBOT in this patient group, and both suggest a trend for improved outcomes in HBOT-treated patients.
HBOT appears to be a potentially attractive option for intervention for those patients with increasing respiratory distress from COVID-19. Supersaturated oxygen can bypass the proposed COVID-related RBC-uploading defect and the pulmonary congestion in these patients and deliver oxygen to hypoxic tissues and organs, thus giving them a “rest” from their hypoxic state.
Also, many of the patients in these two studies demonstrated improved oxygen saturations and decreased hypoxia after completion of treatments, with additional improvements after each additional HBOT intervention. One current hypothesis proposed for this post-treatment clinical improvement is the anti-inflammatory effect of HBOT. [3]
With increasing COVID-19 admissions and increasing morbidity/mortality, HBOT may be an evolving potential intervention for those patients with increasing respiratory distress. It certainly could be considered along with the host of other repurposed “off label’ interventions currently being clinically tasked to treat COVID-19.
Meanwhile, there are eight active or upcoming clinical trials registered on the clinicaltrials.gov website (www.clinicaltrials.gov ) utilizing the search terms “HBOT” and “COVID-19.” Several of these appear to be prospective, randomized efforts. Thus, HBOT might be an evolving clinical option worthy of consideration in this patient population.
References:
- Gorenstein SA, Castellano ML, Slone ES, et al., Hyperbaric oxygen therapy for COVID-19 patients with respiratory distress: treated cases versus propensity-matched controls. Undersea Hyperb Med. Third-Quarter 2020;47(3):405-413.
- Thibodeaux K, Speyrer M, Raza A, et al., Hyperbaric oxygen therapy in preventing mechanical ventilation in COVID-19 patients: a retrospective case series. J Wound Care. 2020 May 1;29(Sup5a):S4-S8. doi: 10.12968/jowc.2020.29.Sup5a.S4.
- Kjellberg A, De Maio A, Lindholm P, Can hyperbaric oxygen safely serve as an anti-inflammatory treatment for COVID-19? Medical Hypotheses 144 (2020) 110224