Queuing theory models offer a telling look at what makes the emergency department grind to a halt
We need to talk more about boarding and ED overcrowding. I know, we’ve been talking about this for decades, and yes, in some ways things are better, but in many places things are worse. From where I stand, overcrowding is still the single most important safety issue facing ED patients nationally. And given the natural demographics of our system – boomers entering retirement, patients living longer with greater disease complexity, increasing emphasis on cost containment – things are likely to get worse unless we keep fighting the trend.
Being a data driven kind of person, and having at my disposal some interesting information from the ED Benchmarking Alliance, it’s easy for me to drill down and see what factors most affect different kinds of EDs – it’s not surprising that urban academic trauma centers have different challenges, and different benchmarks, than rural community EDs.
But sometimes it’s best to avoid diving into the data, and instead think about models that can help explain the challenges EDs are facing. A good model can even show the path toward a solution.
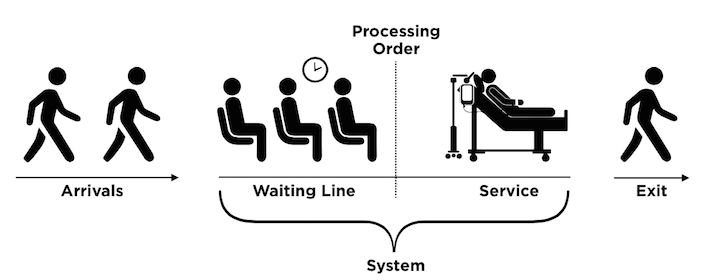
When it comes to crowding, there are many models which can help. The most basic model is to think of the ED as a processing system with inputs, throughputs, and outputs – reminding us that all the elements are connected and if output is blocked, we’ll have backups in the rest of the system. There was a popular model in the 1990s which likened EDs to “clockwork,” and implied the same degree of precision could be engineered into operations. This was a step forward but it was limited because it did not account for the random variability which characterizes health care.
Why is variability so characteristic of health care? We’ve got to remember that EDs are complex systems, with many moving parts and subsystems – from staff to labs to stretchers to workstations – behaving in ways which affect the other parts. Complex systems are like small ecologies; their behavior is non-linear (that is, inputs are often not proportional to outputs), self organizing into smaller systems that are autonomous and constantly exhibiting new behaviors, and therefore always somewhat unpredictable. This unpredictability is best thought of as variability, and it starts from the moment each patient arrives in the ED.
This variability is the source of so much of our trouble when it comes to managing flow. My own best understanding of how powerfully variability can affect flow came when I learned about queuing theory during a course on Lean Operations in Health Care. Queuing theory was developed years ago in business and engineering schools, but only recently have these ideas come to health care, and even later, to the ED.
Queuing brings a powerful set of tools for ED managers, and I would strongly encourage anyone with an interest to learn more. Very likely you have people in your own hospital who have some of these skills. But let me try to summarize the main ideas very quickly.
If you know how many patients are arriving,and you know how many rooms there are, and you know how long each patient stays in the room, then you can calculate how many patients can be seen before a line starts to form. If arrivals were perfectly regular, as the graphic implies, this would be an easy calculation. But as we know, arrivals are not regular; they are in fact more or less random. The math underneath all this is a little tricky, but trust me that the more variability there is in arrivals and each of the subsequent steps, the more inefficient the system becomes and the more likely we are to have backups.
Let’s see what happens when we add in some random variability.
If you remember the shape of the graph below, it will unlock many mysteries as we analyze waiting times and patient flow in the ED. On the Y axis we have waiting time (which can also be converted to number of people waiting); on the X axis, how busy the ED resources are (think of an enzyme receptor site). Is there are linear relationship? Obviously not. Things start to deteriorate at about 85%, and over 90% rapidly approach disaster.

What does this mean in reality? It means you want to match your rooms and staffing to arrivals so you will generally have a little free space, a little slack and extra capacity. Conversely, it means that if you have a surge of arrivals, let’s say 30% over expected, your waiting times will go through the roof. The same thing happens if your treatment spaces are reduced, for instance by RNs calling out sick, the key concept for this discussion, boarding patients. And in the queuing world, once you fall behind, it is really, really hard to catch up.
In our busy ED, given a treatment LOS of about 4 hours for ESI 1/2/3, and knowing the number of arrivals on day shift, we need about 90 rooms open to ensure there are no lines out front. What happens if we have 25 rooms unavailable (essentially closed) due to boarding patients? You guessed it, and it’s not good.
Think for a minute and you will realize that this doesn’t just apply to the overall flow of patients: it also applies to the many, many subsystems within the larger system (e.g. nursing tasks, physician tasks, lab, radiology, transport, registration, flow to the floors, flow through the hospital— each one of these is it’s own mini-queuing system). The interaction between all these sub systems is what generates the extreme complexity of our departments. This is why the concept is so powerful, and worth studying more.
But now that you’ve got a grasp of queuing theory, here are some of the most useful queuing strategies which can be used to help your own situation. Click the image below to view 10 practice ways to address queing concerns.


1 Comment
Charlie,
how are you and the crew at CH?
I miss you guys an hope to visit soon.
Dr Steven Costalas ’97